 Being a pregnant mother for the first time can be nerve wrecking and exciting at the same time. Regular health screening and medical check up helps mothers to have peace of mind knowing their baby is in good condition. This may also help to reduce chances of problems during pregnancy and even if there is any sign of problems, early detection may help healthcare providers to plan treatment or management to minimise the problems. One of the common tools used in evaluating pregnancy is ultrasound.
Being a pregnant mother for the first time can be nerve wrecking and exciting at the same time. Regular health screening and medical check up helps mothers to have peace of mind knowing their baby is in good condition. This may also help to reduce chances of problems during pregnancy and even if there is any sign of problems, early detection may help healthcare providers to plan treatment or management to minimise the problems. One of the common tools used in evaluating pregnancy is ultrasound.
Ultrasound uses high-frequency sound waves to create an image of the baby, placenta and the uterus. It is the safest imaging test used to evaluate a pregnancy as there is no radiation exposure such as in x-rays or CT scan. Ultrasound imaging helps give images from many positions that are not stationary such as in x-rays. It is considered as a special part of the pregnancy journey as this is the first time a mother is able to “see” the baby. In this article, we will be learning more about nuchal translucency and what is normal for it.
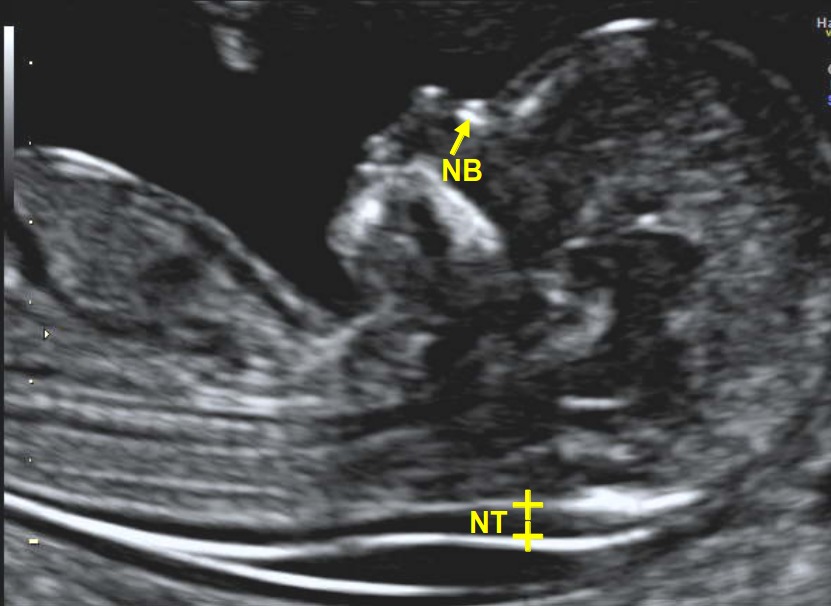
Nuchal translucency is ultrasound that measures appearance of fluid under the skin behind the foetal neck in the first trimester of pregnancy. This is also known as measuring the nuchal fold thickness. Nuchal translucency scan helps to estimate risk for a baby to develop chromosomal abnormality such as Down syndrome and congenital heart problems. Babies with abnormalities tend to accumulate more fluid at the back of the neck during the first trimester.
The question now is, what is considered normal for nuchal translucency? To answer this may not be easy and you may need to ask healthcare providers on how nuchal translucency is measured. Results from nuchal translucency scan usually are not calculated alone. It is typically combined from findings of all first trimester screenings. Results from nuchal translucency scan with the first-trimester or combined sequential screening is presented as mathematical risk. Normal amount of fluid in the back during the ultrasound indicates low chance for congenital condition. Inversely, increased amount of fluid measured compared to the other babies of the same gestational age, would propose higher risk for genetic disorders.
Result of normal and abnormal nuchal translucency is based on the ratio. For example, if the result indicates 1 in 300, meaning that for every 300 babies with the fluid measurement, only one has a congenital condition. Thus, a result of 1 in 1200 would be considered normal because the risk for congenital conditions is lower than 1 in 300. A ratio of 1 in 100 would be considered abnormal because that risk is higher than 1 in 300. Another measurement that can be considered as normal nuchal translucency is measurements of below 2 millimetres at 11 weeks of gestational age and below 2.8 millimetres at 13 weeks of gestational age.
Nuchal translucency screening is a screening test. This means that results cannot guarantee that a baby with normal or abnormal results will or will not have chromosomal abnormality. If results show high risk or abnormal, further tests such as amniocentesis or chorionic villus sampling may be recommended to get definite results. Combination of ultrasound result and blood test can give more accurate estimation risk for up to accuracy of 79 to 90 percent.
It can be concluded that nuchal translucency scans have to be done within the first trimester. Do not panic if the results show abnormal results. Remember, it is a screening test and not a definite test that would confirm a baby does have congenital abnormalities. It is important to discuss with healthcare providers on what to do next and the real meaning of the test results.
Also read – Dengue Prevention.


